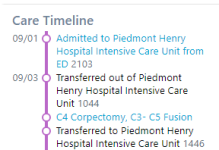
A hospital we are affiliated with and perform ED, Observation, and Inpatient services with has placed a patient in Inpatient status too early for the service I am coding and billing for to be covered by the patient's insurance.
The patient was listed by the hospital as being in Inpatient status, but my manager is telling me to code it and POS as Emergency Department instead. I don't believe this would be correct coding or billing just so we get the service covered and paid for. Who is right here in this scenario?
The patient was listed by the hospital as being in Inpatient status, but my manager is telling me to code it and POS as Emergency Department instead. I don't believe this would be correct coding or billing just so we get the service covered and paid for. Who is right here in this scenario?