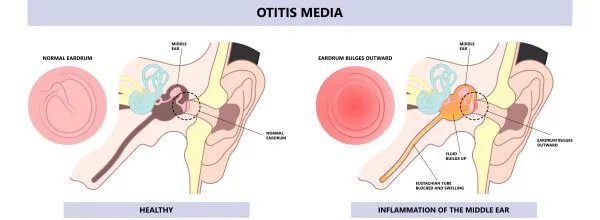
Defer to Provider for Otitis Media Timeline Guidance
Question: My otolaryngologist documented otitis media with effusion for one patient and chronic otitis media with effusion for another What is the difference, and how do I code them? Arizona Subscriber Answer: The key difference between these two ailments is simply the duration of the effusion. But defining what is acute and what is chronic itself is not so simple. Otitis media with effusion (OME), also known as serous OM, is swelling and fluid buildup (effusion) in the middle ear without signs of an acute bacterial or viral infection and can occur following an episode of acute otitis media (AOM). The ICD-10-CM Alphabetic Index tells you to look to Otitis, media, nonsuppurative to find otitis (acute) with effusion, which leads you to H65.9- (Unspecified nonsuppurative otitis media). Here, you’ll see the synonym “otitis media with effusion (nonpurulent) NOS,” confirming you have the right code for the condition. Chronic otitis media with effusion (COME) occurs when fluid (effusion) remains in the middle ear for a long time or builds up repeatedly, even though there is no infection. For this condition, the index tells you to go to Otitis, media, nonsuppurative, chronic, which leads you to use H65.49- (Other chronic nonsuppurative otitis media). Here, you’ll see the synonym “chronic otitis media with effusion (nonpurulent),” confirming you have the right code for the condition. Note: ICD-10-CM Official Guideline I.B.8, “Acute and Chronic Conditions,” doesn’t provide a definitive timeframe for what makes a condition chronic or acute, and external definitions are also not definitive. CPT® guidelines for evaluation and management (E/M) coding, for example, list a stable, chronic illness as “a problem with an expected duration of at least one year or until the death of the patient,” while an acute problem is generally defined as a “recent or new short-term problem.” And the Centers for Disease Control and Prevention (CDC) defines chronic conditions as those “that last 1 year or more and require ongoing medical attention or limit activities of daily living or both.” Consequently, whether a condition is defined as acute or chronic comes down to your provider’s judgment. If your provider’s documentation lists acute or chronic, then that is how you will determine your code assignment. If your provider’s documentation does not specify, then you should consider querying the provider to clarify which it is from their perspective. Bruce Pegg, BA, MA, CPC, CFPC, Managing Editor, AAPC